




































Study with the several resources on Docsity

Earn points by helping other students or get them with a premium plan


Prepare for your exams
Study with the several resources on Docsity

Earn points to download
Earn points by helping other students or get them with a premium plan
Community
Ask the community for help and clear up your study doubts
Discover the best universities in your country according to Docsity users
Free resources
Download our free guides on studying techniques, anxiety management strategies, and thesis advice from Docsity tutors
ACLS Exam Version A&B questions and answers 2023/24 latest 100% CORRECT Already Passed., Exams of Nursing
Typology: Exams
1 / 45

This page cannot be seen from the preview
Don't miss anything!






































A
Advanced Cardiovascular Life Support Exam Version A ( questions) Please do not mark on this exam. Record the best answer on the separate answer sheet.
1. You find an unresponsive patient who is not breathing. After activating the emergency response system, you determine that there is no pulse. What is your next action? A. Open the airway with a head tilt–chin lift. B. Administer epinephrine at a dose of 1 mg/kg. C. Deliver 2 rescue breaths each over 1 second. D. Start chest compressions at a rate of at least 100/min. 2. You are evaluating a 58-year-old man with chest pain. The blood pressure is 92/50 mm Hg, the heart rate is 92/min, the nonlabored respiratory rate is 14 breaths/min, and the pulse oximetry reading is 97%. What assessment step is most important now? A. PETCO 2 B. Chest x-ray C. Laboratory testing D. Obtaining a 12-lead ECG 3. What is the preferred method of access for epinephrine administration during cardiac arrest in most patients? A. Intraosseous B. Endotracheal C. Central intravenous D. Peripheral intravenous
A
4. An activated AED does not promptly analyze the rhythm. What is your next action? A. Begin chest compressions. B. Discontinue the resuscitation attempt. C. Check all AED connections and reanalyze. D. Rotate AED electrodes to an alternate position.
A
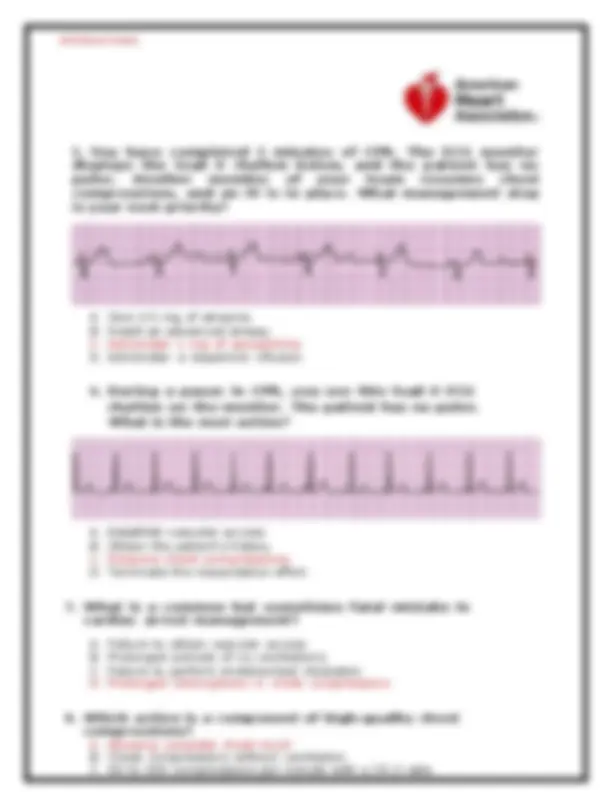
5. You have completed 2 minutes of CPR. The ECG monitor displays the lead II rhythm below, and the patient has no pulse. Another member of your team resumes chest compressions, and an IV is in place. What management step is your next priority? A. Give 0.5 mg of atropine. B. Insert an advanced airway. C. Administer 1 mg of epinephrine. D. Administer a dopamine infusion. 6. During a pause in CPR, you see this lead II ECG rhythm on the monitor. The patient has no pulse. What is the next action? A. Establish vascular access. B. Obtain the patient’s history. C. Resume chest compressions. D. Terminate the resuscitative effort. 7. What is a common but sometimes fatal mistake in cardiac arrest management? A. Failure to obtain vascular access B. Prolonged periods of no ventilations C. Failure to perform endotracheal intubation D. Prolonged interruptions in chest compressions 8. Which action is a component of high-quality chest compressions? A. Allowing complete chest recoil B. Chest compressions without ventilation C. 60 to 100 compressions per minute with a 15:2 ratio
A D. Uninterrupted compressions at a depth of 1½ inches
A D. detects electrolyte abnormalities early in code management.
A
14. For the past 25 minutes, an EMS crew has attempted resuscitation of a patient who originally presented in ventricular fibrillation. After the first shock, the ECG screen displayed asystole, which has persisted despite 2 doses of epinephrine, a fluid bolus, and high-quality CPR. What is your next treatment? A. Apply a transcutaneous pacemaker. B. Administer 1 mg of intravenous atropine. C. Administer 40 units of intravenous vasopressin. D. Consider terminating resuscitative efforts after consulting medical control. 15. Which is a safe and effective practice within the defibrillation sequence? A. Stop chest compressions as you charge the defibrillator. B. Be sure oxygen is not blowing over the patient’s chest during the shock. C. Assess for the presence of a pulse immediately after the shock. D. Commandingly announce “clear” after you deliver the defibrillation shock. 16. During your assessment, your patient suddenly loses consciousness. After calling for help and determining that the patient is not breathing, you are unsure whether the patient has a pulse. What is your next action? A. Leave and get an AED. B. Begin chest compressions. C. Deliver 2 quick ventilations. D. Check the patient’s mouth for the presence of a foreign body. 17. What is an advantage of using hands-free defibrillation pads insteadof defibrillation paddles? A. Hands-free pads deliver more energy than paddles. B. Hands-free pads increase electrical arc. C. Hands-free pads allow for a more rapid defibrillation. D. Hands-free pads have universal adaptors that can work with any machine. 18. What action is recommended to help minimize interruptions in chest compressions during CPR? A. Continue CPR while charging the defibrillator. B. Perform pulse checks immediately after defibrillation.
A D. Preparation for therapeutic hypothermia
A
20. Which drug and dose are recommended for the management of a patient in refractory ventricular fibrillation? A. Atropine 2 mg B. Amiodarone 300 mg C. Vasopressin 1 mg/kg D. Dopamine 2 mg/kg per minute 21. What is the appropriate interval for aninterruption in chest compressions? A. 10 seconds or less B. 10 to 15 seconds C. 15 to 20 seconds D. Interruptions are never acceptable 22. Which of the following is a sign of effective CPR? A. PETCO 2 ≥10 mm Hg B. Measured urine output of 1 mL/kg per hour C. Patient temperature >32°C (89.6°F) D. Diastolic intra-arterial pressure <20 mm Hg 23. What is the primary purpose of a medical emergency team(MET) or rapid response team (RRT)? A. Identifying and treating early clinical deterioration B. Rapidly intervening with patients admitted through emergency department triage C. Responding to patients during a disaster or multiple-patient situation D. Responding to patients after activation of the emergency response system 24. Which action improves the quality of chest compressions delivered during a resuscitation attempt? A. Observe ECG rhythm to determine depth of compressions. B. Do not allow the chest to fully recoil with each compression. C. Compress the upper half of the sternum at a rate of 150 compressions per minute. D. Switch providers about every 2 minutes or every 5 compression cycles. 25. What is the appropriate ventilation strategy for an adult in respiratory arrest with a pulse rate
A D. 2 breaths every 6 to 8 seconds
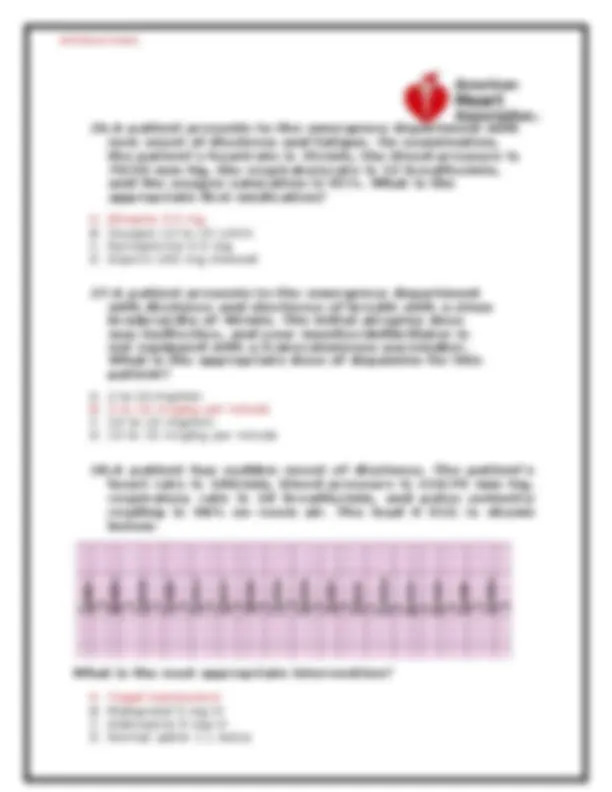
A 26.A patient presents to the emergency department with new onset of dizziness and fatigue. On examination, the patient’s heartrate is 35/min, the blood pressure is 70/50 mm Hg, the respiratoryrate is 22 breaths/min, and the oxygen saturation is 95%. What is the appropriate first medication? A. Atropine 0.5 mg B. Oxygen 12 to 15 L/min C. Epinephrine 0.5 mg D. Aspirin 160 mg chewed 27.A patient presents to the emergency department with dizziness and shortness of breath with a sinus bradycardia of 40/min. The initial atropine dose was ineffective, and your monitor/defibrillator is not equipped with a transcutaneous pacemaker. What is the appropriate dose of dopamine for this patient? A. 2 to 10 mg/min B. 2 to 10 mcg/kg per minute C. 10 to 15 mg/min D. 10 to 15 mcg/kg per minute 28.A patient has sudden onset of dizziness. The patient’s heart rate is 180/min, blood pressure is 110/70 mm Hg, respiratory rate is 18 breaths/min, and pulse oximetry reading is 98% on room air. The lead II ECG is shown below: What is the next appropriate intervention? A. Vagal maneuvers B. Metoprolol 5 mg IV C. Adenosine 6 mg IV D. Normal saline 1 L bolus
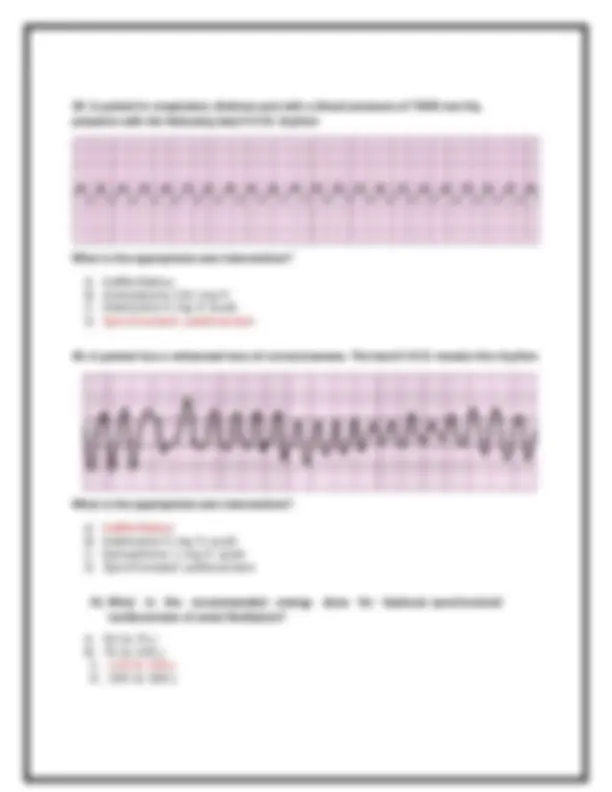
A 29.A monitored patient in the ICU developed a sudden onset of narrow-complex tachycardia at a rate of 220/min. The patient’s blood pressure is 128/58 mm Hg, the PETCO 2 is 38 mm Hg, and the pulse oximetry reading is 98%. There is vascular access at the left internal jugular vein, and the patient has not been given any vasoactive drugs. A 12-lead ECG confirms a supraventricular tachycardia with no evidence of ischemia or infarction. The heart rate has not responded to vagal maneuvers. What is the next recommended intervention? A. Adenosine 6 mg IV push B. Amiodarone 300 mg IV push C. Synchronized cardioversion at 50 J D. Synchronized cardioversion at 200 J 30.You are receiving a radio report from an EMS team en route with a patient who may be having an acute stroke. The hospital CT scanner is not working at this time. What should you do in this situation? A. Contact the patient’s family to see what they would prefer. B. Have the EMS crew choose an appropriate patient disposition. C. Accept the report and provide care within your present capability. D. Divert the patient to a hospital 15 minutes away with CT capabilities. 31.Choose an appropriate indication to stop or withhold resuscitative efforts. A. Arrest not witnessed B. Evidence of rigor mortis C. Patient age greater than 85 years D. No return of spontaneous circulation after 10 minutes of CPR 32.A 49-year-old woman arrives in the emergency department with persistent epigastric pain. She had been taking oral antacids for the past 6 hours because she thought she had heartburn. The initial blood pressure is 118/72 mm Hg, the heart rate is 92/min and regular, the nonlabored respiratory rate is 14 breaths/min, and the pulse oximetry reading is 96%. Which is the most appropriate intervention to perform next? A. Administer oxygen. B. Obtain a 12-lead ECG. C. Evaluate for fibrinolytic eligibility. D. Administer sublingual nitroglycerin. 33.A patient in respiratory failure becomes apneic but
A continues to have a strong pulse. The heart rate is dropping rapidly and now shows a sinus bradycardia at a rate of 30/min. What intervention has the highest priority?
A 34.What is the appropriate procedure for endotracheal tube suctioning after the appropriate catheter is selected? A. Suction during insertion but for no longer than 30 seconds. B. Suction the mouth and nose for no longer than 30 seconds. C. Suction during withdrawal but for no longer than 10 seconds. D. Hyperventilate before catheter insertion, and then suction during withdrawal. 35.While treating a patient with dizziness, a blood pressure of 68/30 mm Hg, and cool, clammy skin, you see this lead II ECG rhythm: What is the most appropriate first intervention? A. Aspirin B. Atropine C. Lidocaine D. Nitroglycerin 36.A 68-year-old woman experienced a sudden onset of right arm weakness. EMS personnel measure a blood pressure of 140/90mm Hg, a heart rate of 78/min, a nonlabored respiratory rate of 14 breaths/min, and a pulse oximetry reading of 97%. The lead II ECG displays sinus rhythm. What is the most appropriate action for the EMS team to perform next? A. 12-lead ECG assessment B. Administration of 100% supplementary oxygen C. Cincinnati Prehospital Stroke Scale assessment D. Administration of a low-dose aspirin 37.EMS is transporting a patient with a positive prehospital stroke assessment. Upon arrival in the emergency department, the initial blood pressure is 138/78 mm Hg, the pulse rate is 80/min, the respiratory rate is 12 breaths/min, and the pulse oximetry reading is 95% on room air. The lead II ECG displays sinus rhythm. The blood glucose level is within normal limits. What intervention should you perform next?
A A. Head CT scan B. Transfer to the stroke unit C. Immediate rtPA administration D. Administration of 100% oxygen